Article
Helping IDNs improve clinical and economic outcomes in pursuit of value-based care
Healthcare isn’t truly optimized until everyone is working from the same page. Providers operate more efficiently when communication is clear and consistent. Patients have confidence when they know all their healthcare providers are closely aligned. However, too often, patients experience disparate treatment as they move from one stage of the care journey to the next — and these discrepancies can create confusion; redundancy and waste; the potential for mistakes; and possibly mistrust. There is a strong need for dependable, value-based care implemented across the board. By prioritizing quality of care over quantity of treatments, value-based care rewards effectiveness and efficiency — ultimately improving overall patient experiences and the bottom line.
The origins of this shift toward value-based care can be found in the passage of the Affordable Care Act, which spurred the growth of Integrated Delivery Networks (IDNs) and amplified the call for access to lower-cost care settings like home health. This, along with the continuing growth of the geriatric population has resulted in more and more patients receiving home or outpatient treatment for chronic conditions such as wound care.
As the largest healthcare organizations in the country, IDNs play a key role in supporting this movement. But while many IDNs have come to appreciate the benefits of value-based care, few have taken steps to implement this model across the entire patient journey — also known as the continuum of care.
Today, lack of consistency in care represents a major issue for IDNs. Managing dozens of hospitals and healthcare facilities, IDNs know that value-based care doesn’t stop at discharge, and that the care process is rarely linear. However, a lack of communication and standardization throughout networks remains an obstacle to achieving the ultimate purpose of the IDN: efficiency, value and optimization of care.
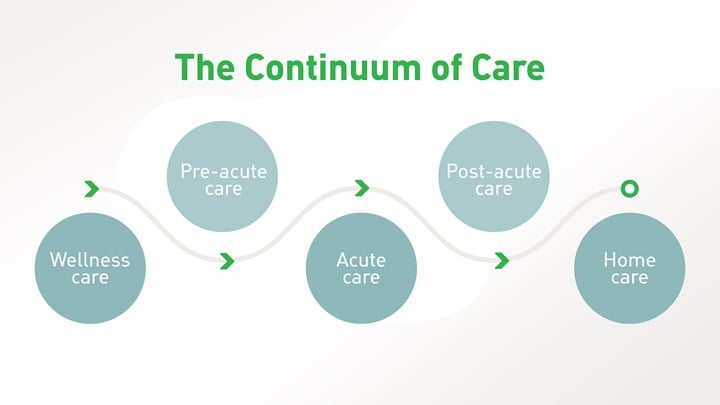
Where the care continuum breaks down impacting value-based care
Each transition between healthcare settings is an opportunity for gaps and possible failure points that can significantly impact patient outcomes. With so many people involved in a real-world care setting — from physicians, nurses and care assistants to discharge planners, social workers and so on — each movement in the patient journey can potentially rely on a different decision maker or caregiver operating under different protocols with a different level of experience. As such, ensuring that acute and post-acute care plans are properly communicated and adhered to is paramount to maintain consistency.
Variation in products and protocols represents another potential failure point in the patient journey. In order to maximize total value throughout the continuum of care, IDNs must ensure consistent product quality and patient experience in every healthcare setting to achieve value-based care at scale. Failure to do so creates opportunity for human error and poorer outcomes, as well as patient confusion and anxiety. Standardization in products and protocols helps promote seamless transitions across the continuum of care and supports total value for both patients and providers.
“When it comes to human error, if you give someone one item to choose from, they will choose that item 100% of the time. But if you give them 25 items to choose from, it opens up a huge risk for error.”
— Sam Sullivan, RN, CNOR and a Lean expert at Strong Memorial Hospital in New York.1
Inconsistent care leads to inconsistent outcomes
This lack of communication, coordination and consistency has the potential to seriously jeopardize value-based care for IDNs. Without standardization throughout the patient journey, IDNs face challenges collecting reliable data to improve best practices. As a result, failure points in the continuum of care may go unnoticed or unaddressed for extended periods, leading to adverse results such as
- longer patient stays
- higher readmission rates
- and poorer patient outcomes.
Product standardization removes one of the major variables in assessing patient outcomes, helping IDNs maximize total value across the patient journey and ensure top care standards are maintained.

Inconsistent outcomes drain hospital resources
Over the last decade, CMS has implemented multiple programs which associate reimbursement penalties with facility performance. This is designed to incentivize better patient care and provide guardrails against poor outcomes. Naturally wound care has emerged as a top priority, given that pressure injuries, HAIs and excessive readmissions are closely watched by CMS.2,3 In February 2022, CMS announced it is imposing penalties to 764 hospitals due to their HAI rates, resulting in a 1% reduction in their Medicare payments over 12 months.4 In 2021, 82% of hospitals evaluated for readmission rates received CMS penalties, costing hospitals an estimated $521 million.5
Aside from CMS penalties for poor performance, patients with multiple co-morbidities are simply more expensive to treat. Inconsistent care may result in more complex case mixes — which require a disproportionate share of healthcare resources. The correlating costs can be significant, impacting areas such as physician access, nursing overtime and medical supplies. Pressure injuries, for example, are estimated to account for nearly $43,180 per incidence in additional treatment costs to a hospital stay. Given that these preventable injuries are the second most common source of lawsuits in the healthcare industry behind wrongful death, a standardized, value-based care approach offers substantial opportunity for cost savings and improved outcomes.6
It’s time to look at healthcare holistically through the Total Value lens
By implementing a value-based approach across the continuum of care, IDNs can see:
Clearer measurements
Standardized products and practices help promote consistent experiences and results. Consistent results provide IDNs with more reliable data that can be used to pinpoint and rectify training gaps, generate new best practices and improve efficiency throughout their facilities.
Improved clinical outcomes
Formalizing communication and care protocols throughout the patient journey will go a long way to preventing skipped steps and bedside “guesses.” When clinicians have clear guardrails and best practices to follow, there is less chance for error — and differences in clinician education levels become less paramount. All of this sets the stage to decrease readmissions, improve quality metrics and increase overall ratings.
The largest rural hospital in the U.S. nearly doubled their 16-week wound healing rate by standardizing wound care products and practices. As a result, wound care patient satisfaction rates increased 13%, and clinical satisfaction rose as well.7
Enhanced clinical acumen
Standardizing protocols and products allow IDNs to reinforce best practices across the continuum of care — improving both patient outcomes and clinician performance.
- Reduced training time: With everyone on the same page, the training process can be streamlined. Education is one area of standardization that is key to helping produce better outcomes at a lower cost.8
- Increased clinician efficiency: Clinicians can work more efficiently when they can count on using the same products every time, no matter what hospital area or facility they’re in.
- Improved clinical safety: Healthcare workers may interact with thousands of products each day, leading to confusion and mistakes. Standardizing products can help prevent workplace injuries from common sources like patient handling, needle sticks and infection exposure.9
A connected acute/post-acute network
When post-acute providers develop partnerships with healthcare networks, they typically come with their own way of doing things. Allowing post-acute facilities to continue their pre-established protocols may offer the path of least resistance, but this laissez-faire approach ultimately harms both patient outcomes and network operations. By closing the gaps between acute care and post-acute care through standardization, IDNs can improve clinical outcomes through shared and informed decision-making.
Greater purchasing power
Standardizing specific patient care products across multiple lines of service or facilities can streamline inventory and reduce waste — resulting in substantial savings.
- Simplified supply chains: The average hospital manages around 8,000 SKUs of inventory in-house alone, with up to 35,000 SKUs on the product formulary.10 A streamlined inventory reduces the complexity of logistics and helps ensure a consistent supply of quality products.
- Improved pricing with higher volume: IDNs already know the benefits of bulk purchasing for hospitals. Between 2016 and 2020, surgical supply expenses increased 5% for IDN-owned hospitals, compared to 5.7% for independent entities.11 By expanding this practice and purchasing products as a healthcare system rather than as individual entities, IDNs can leverage order volume to maximize buying power.
- Reduced redundancy and increased efficiency: With fewer SKUs to manage, IDNs can more effectively oversee existing contracts and streamline vendor relations.

Implementing total value across the continuum of care
It is clear that a harmonized approach across all care settings results in better performance across the board. By standardizing best practices and ensuring alignment between acute and post-acute care, IDNs can create opportunity for significant improvement in health and financial outcomes.
Mölnlycke provides solutions tailored to the most pervasive issues within the continuum of care, including pressure injury management, standardization, and infection prevention — to help IDNs identify and close gaps in care within the patient journey. By working to address these common failure points across all healthcare settings, IDNs can improve patient outcomes, reduce waste of facility resources, and achieve total value across the continuum of care.12
References
- Mölnlycke Health Care white paper, “Standardization is Key to Maximizing the Total Value of Patient Care Products,” 2021
- Centers for Medicare and Medicaid Services, “Hospital Readmissions Reduction Program (HRRP),” accessed June 2022
- Centers for Medicare and Medicaid Services, “Hospital-Acquired Condition Reduction Program,” accessed June 2022
- Jordan Rau, “Health Care Paradox: Medicare Penalizes Dozens of Hospitals It Also Gives Five Stars,” Kaiser Health News, February 8, 2022
- Jordan Rau, “Medicare Punishes 2,499 hospitals for High Readmissions,” Kaiser Health News, October 28, 2021
- Agency for Healthcare Research and Quality, “Preventing Pressure Ulcers in Hospitals,” accessed May 2022
- McNees, Patrick, and John A. Kueven. "The bottom line on wound care standardization: at North Mississippi Medical Center, standardization of wound care processes and products led to improved healing rates and a $300,000 annual reduction in supply expenses." Healthcare Financial Management, vol. 65, no. 3, Mar. 2011, pp. 70+.
- McNees, Patrick, and John A. Kueven. "The bottom line on wound care standardization: at North Mississippi Medical Center, standardization of wound care processes and products led to improved healing rates and a $300,000 annual reduction in supply expenses." Healthcare Financial Management, vol. 65, no. 3, Mar. 2011, pp. 70+.
- Harding K, Black J, Gefen A, Santamaria N, Alves P, Ohura N, Bindle T, Trevellini C. Meeting report: Are you doing everything possible to prevent pressure injury throughout the patient’s hospital stay? Wounds International 2016 | Vol 7 Issue 4 | pg 37-43
- Mullins D, MBA, CMRP, Persaud EJ, Ferko NC, Knight B, Tripodi D, Delatore P. “SKU Optimization Initiatives Can Create Cost Savings in an Era of Value-Based Care.” Healthcare Financial Management Association, January 31, 2019
- Definitive Healthcare, “Annual changes in hospital medical supply costs,” accessed May 2022
- Kalowes P., Messina V. et al. Five-layered soft silicone foam dressing to prevent pressure ulcers in the intensive care unit. Am J of Critical Care 2016; 25: 6, 108-119




